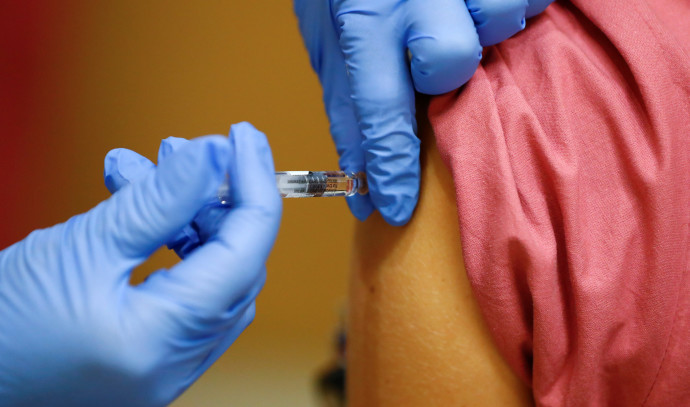
Sometimes people go to their health fund clinic for more than one vaccination at a time – flu, shingles, COVID-19, tetanus and more. But many doctors and even nurses don’t know the answer to the “trivial” question – should the shot be given in different arms or the same one.
“The question seems so banal that nobody before has thought to ask it,” said transplant and infection immunology Prof. Martina Sester of Saarland University in Germany, who sought the answer with her doctoral student Laura Ziegler.
The two just published their study in the journal EBioMedicine under the title “Differences in SARS-CoV-2 specific humoral and cellular immune responses after contralateral and ipsilateral COVID-19 vaccination.”
Sester and Ziegler, who are interested in examining the effectiveness of vaccinations, are far more likely to ask questions like how does the vaccine move through the body? Does it travel directly or indirectly to the target site, and does it do any damage to normal body cells on the way? Is this vaccine more effective than that one, and which has the longer immune response? But so far no one has addressed the simple question of whether it’s better for a doctor or nurse to give sequential vaccination shots in the same arm or to deliver one in the left arm and one in the right.
That may now be about to change.
“Both ipsilateral [on one side] and contralateral [on both sides] vaccination induce a strong immune response, but secondary boosting is more pronounced when choosing vaccine administration-routes that allows for drainage by the same lymph nodes used for priming. Our study indicates that ipsilateral vaccinations generate a stronger immune response than contralateral vaccinations,” the 23-year-old Ziegler explained.
Study looked at 303 people from Germany
Germany’s COVID-19 vaccination campaign provided an ideal setting for the two researchers to study this question.
They created a reliable dataset of 303 people who received the mRNA vaccine from Biontech as their primary and booster shots at the start of Germany’s COVID-19 vaccination campaign. The most striking result was that two weeks after the booster shot the number of cytotoxic CD8+ T cells, often referred to as “killer T cells,” was significantly higher in those who had been injected in the same arm.
“In the ipsilateral subjects, we were able to detect the killer T cells in 67% of cases, but we detected CD8+ T cells in only 43% of the contralaterally vaccinated subjects,” Ziegler noted. That may suggest that that ipsilateral vaccination is more likely to provide better protection if the vaccinated person becomes infected with the SARS-CoV-2 virus.
“The number of antibodies, however, was not greater,” added Sester.
Unlike the killer cells, the antibodies do not immediately destroy the virus. Instead, they dock onto the virus preventing it from causing further harm or making it easier for macrophages to find the virus and then engulf and degrade it. What’s interesting is that the antibodies in the ipsilaterally vaccinated subjects were better at binding to the viral spike protein. So the antibodies in those persons who were vaccinated in the same arm were better at doing their job than the antibodies in those who were given injections in both arms.
So far there have been hardly any studies looking into the significance of where primary and booster vaccination shots are applied.
“As dramatic as the pandemic was, it has provided us with reliable data that enables us to address questions of this kind,” Sester explained.
As she analyzed data only from individuals who had received two shots of the Biontech SARS-CoV-2 vaccine, the 23-year-old doctoral student researcher is suitably cautious about generalizing the conclusions of her study.
“Further work is required before we know whether the study has implications for other sequential vaccinations such as those to protect against the flu or tropical diseases. But it does seem possible that some vaccinations will generate a stronger immune response if the injections are delivered into the same arm – making the apparently naive question posed at the beginning of the study suddenly seem not quite so banal after all.”