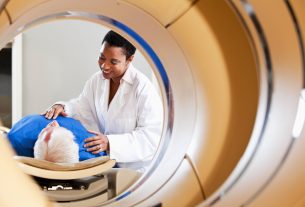
Belgian AI company Kantify was doing business as usual until a cancer diagnosis forced the team to rethink their direction. “We built algorithms for sectors like marketing or transport,” said Ségolène Martin, Kantify’s co-founder and CEO.
“Those were complex projects that had nothing to do with health, but they enabled us to build a deep expertise in AI.”
That changed in 2017, when Nik Subramanian, the company’s CTO, was diagnosed with sarcoma, a rare type of cancer that forms tumours in connective tissues such as bones, muscles and blood vessels.
This experience prompted the company to shift its focus to health and explore the potential of AI to help improve how new drugs for rare diseases are identified and tested.
“It changed our lives,” said Martin. “We are now completely focused on AI for human health, and have developed a specialised technology for AI-based drug discovery.”
That expertise is now being fully used as part of a five-year EU‑funded research initiative called DREAMS. It is focused on improving treatments for a group of five rare neuromuscular disorders that progressively weaken muscle function.
Increasing the odds for patients
“
We are now completely focused on AI for human health, and have developed a specialised technology for AI-based drug discovery.
Developing treatments for rare diseases remains one of the biggest challenges in modern medicine. The process is long, expensive and uncertain, requiring years of research, regulatory approval and clinical trials.
For pharmaceutical companies, the small number of patients often makes such investments difficult to justify. As a result, many conditions remain untreated.
Today, only around 5–6% of the estimated 7 000 to 10 000 rare diseases have an approved therapy, a gap that organisations such as the World Health Organization continue to highlight as a global priority.
AI could help change that. By rapidly analysing vast datasets, AI can narrow down potential drug candidates at an early stage and identify existing medicines that might be repurposed for rare conditions.
A focus on neuromuscular disorders
Within DREAMS, researchers are focusing on five rare neuromuscular disorders, including Duchenne muscular dystrophy, which primarily affects young boys and causes muscle degeneration, and Emery–Dreifuss muscular dystrophy, which can cause severe heart issues.
Although these conditions differ in their genetic causes, they appear to share underlying mechanisms of action at the cellular level. By targeting these common pathways, researchers hope to develop treatments that could benefit several diseases at once, rather than tackling each one separately.
To do this, the team reprogrammes patient cells into so-called induced pluripotent stem cells (iPSCs) – a type of master cell that can be turned into many other cell types – and then turns them into skeletal muscle tissue. This allows researchers to study the disease in a controlled setting.
By combining these lab models with AI, researchers can identify shared therapeutic targets across multiple conditions.
“This kind of research is crucial for patients and their families,” said Xavier Nissan, project coordinator of DREAMS and research director at French research institute I‑Stem that specialises in stem cell therapy and the treatment of monogenic diseases.
“They are suffering and have to deal with their disease every day. They need technology like this.”
From data to potential treatments
As well as identifying the underlying disease processes, the DREAMS researchers are using AI to analyse billions of new and existing drugs, to try and predict which compounds are most likely to work.
“This is one of the ways in which AI can generate real societal value,” said Martin. “It can truly accelerate research and create impact in areas where progress has been slow.”
In the lab, the team is testing a library of 2 700 EMA‑ and FDA‑approved drugs to assess whether any of them could improve shared disease-related symptoms.
“In the lab, we test thousands of existing drugs on iPSC-derived muscle cells from patients with these diseases,” said Nissan.
“AI is then also used to understand how the drugs might work, identify targets, and even predict additional diseases where the treatment could be useful. By combining these approaches, we can move faster and focus on the most promising candidates.”
The team has spent three years generating the data to feed the AI and enable these predictions for drug repurposing.
Central to this drug search is Sapian, Kantify’s AI platform. It is trained on a large amount of data, ranging from information on molecules and proteins to patents and characteristics of all kinds of drugs. Based on this information, the platform can predict which drugs might be good candidates for certain kinds of diseases.
“It’s not a crystal ball,” said Martin. “It will generate hypotheses that will need to be tested in the real world. However, from different projects we have learned that the hypotheses are extremely good.”
In the same basket
It is still unclear when we can expect this approach to yield new treatments for people with rare diseases. Nissan is cautious, pointing to a lot of factors at play and not wanting to give false hope to patients living with these conditions today.
“The project concludes at the end of 2028. Beyond that, there is a big question mark. We are doing our best, but in the world of drugs, things can take a long time.”
Much will depend on what happens when these approaches are tested on patients. New drugs sometimes take decades to complete clinical trials, and even existing drugs that have already passed through these processes will still need to go through some trials.
“
We have a chance to make a big difference in the lives of a lot of people. That’s a beautiful thing to work on.
The DREAMS team is working to make some of these trials more feasible for rare diseases. One problem they encounter is that there are not enough people living with these diseases to do large enough clinical trials.
The researchers are therefore suggesting an alternative approach. “Some rare diseases have wildly different symptoms, but share biological causes,” said Nissan.
“This is why we want to do so-called basket trials, where one drug is tested on people with different symptoms and diseases that share a similar cause,” he said.
This approach, led by patient association AFM‑Téléthon and the patients themselves, could help speed up drug development for people with rare diseases.
Regulatory agencies are now exploring the broader adoption of basket clinical trial approaches for rare diseases, Nissan said.
For Nissan and Martin, this work is more than research. It is personal.
“The patients need us,” said Nissan. “That’s a huge responsibility. I feel I need to succeed. But that also means we have a chance to make a big difference in the lives of a lot of people. That’s a beautiful thing to work on.”
Research in this article was funded by the EU’s Horizon Programme. The views of the interviewees don’t necessarily reflect those of the European Commission. If you liked this article, please consider sharing it on social media.