It’s another tragic record. A new report has confirmed yet another rise in drug related deaths in England and Wales. The Office for National Statistics (ONS) reports that 4,907 “drug poisoning” deaths were recorded in 2022 (84.4 deaths per 1,000,000 of the population), the highest on record.
While there was a slight fall in deaths in men (from 3,275 in 2021 to 3,240 in 2022), this was masked by a corresponding increase in women (from 1,584 in 2021 to 1,667 in 2022). This reflects a longer term trend of females catching up with male mortality. Drug-related suicides, a topic that doesn’t usually receive much attention in discussions about drug-related harms, were also higher in women than men.
Most deaths involved multiple substances, however opiates were detected in just under half of all deaths (2,261 cases).
Of concern are cocaine deaths (857 cases), which have now increased for 11 consecutive years. It’s not possible to determine whether these related to use of powder or crack cocaine. But we know there’s been an increase in the use of cocaine as well as a boost in the global production, supply, purity, affordability and availability of the drug, despite frequent large seizures by law enforcement agencies.
Cocaine has become more potent and more affordable in recent years. Both factors increase the risk of harm including fatal overdose. We’ve also lagged behind developing support for people who use cocaine compared to those who use opioids.
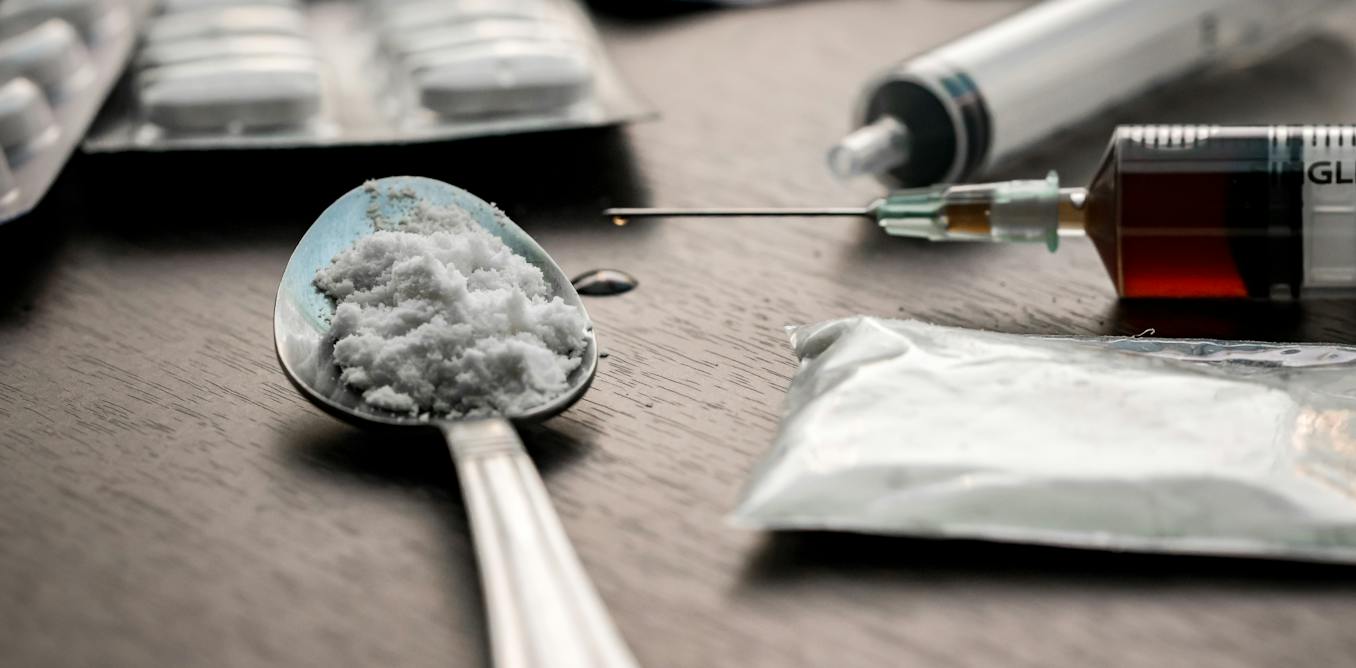
DFree/Shutterstock
Surprisingly, despite its popularity in recreational settings, ketamine is not included in the data – and it is unclear why. Other research suggests there are around 30 deaths each year in England, which is lower than the number of ecstasy deaths (50 in 2022), despite being used by more people.
As for fentanyl, there were tens of thousands of deaths in the US each year. However, in England and Wales these have remained low (57) and stable.
That’s reassuring, but it’s important not to be complacent. There has been recent concern about the emergence of other types of even more potent opioids, with many experts predicting that these drugs will become more prevalent if opium production in Afghanistan continues to decline – leading to fears of even greater increases in drug deaths.
There were also sharp geographical differences in death rates, with those in more deprived areas in the north east and north west of England much higher than other areas. While there were higher rates of opioid and crack use in these regions, this also reflects wider health and social inequalities.
Age as a risk factor
The highest rate of deaths occurred in the 40- to 49-year-old age group, and the average age at death continued to rise. This is mainly the “Generation X” cohort born in the 1970s, who came of age when there was a rapid rise in the availability of heroin, and when general population rates of drug use were at their highest in the 1990s.
These premature deaths reflect poorer physical and psychological health, such as compromised respiratory and cardiovascular functioning, which increases the risk of dying from drugs. Many of these health problems could be treated if people accessed health services, but unfortunately too few do – adding to the risk of premature death.
The data doesn’t reveal everything though. It is also possible that coroners may record a physical health issue as the cause of death, rather than use of drugs. This adds to an underestimation of the number of people dying from drugs.
Synthetic opioids, implicated in local spikes in deaths, aren’t fully captured in the latest ONS figures either. This is because there are delays between when a death occurs, when it is officially recorded by the coroner and when it is included in ONS reports. The latest report includes deaths which occurred in 2021 and 2022, and even as far back as 2017.
While rapid response investigatory panels have been set up in some local areas, these continuing delays hinder rapid assessment of threats to public health.
It may seem paradoxical that overall drug use is declining while drug-related deaths are rising. But this can be explained by the time taken to develop dependent use of drugs and the accompanying problems and risk to health.
Reversing fatalities
The government commissioned Dame Carol Black to advise on how the record number of drug related deaths could be reversed. Her report, published in 2020 and 2021, provided several suggestions including increasing investment in drug treatment which the government has accepted.
While provision of evidence-based drug treatment reduces the risk of death, increased investment will take time to have an impact. It comes after a decade of austerity, which severely affected provision of drug services. Currently, only about half of people who might benefit from formal support are accessing treatment services.
There is no single intervention that will reduce death rates, and the complex profile of the illicit drug market and the cocktail of drugs implicated in deaths means that a whole systems response is required. Most importantly, recent uplifts in funding of treatment services need to be maintained. This will be challenging given the economic pressure on public services.
The priority should be an increase in the community provision of naloxone, the opioid overdose reversal drug. This can already be distributed through drug services, and an increasing number of police officers are also carrying it. Supervised drug consumption facilities, such as the one due to be trialled in Glasgow in 2024 may reduce risks in some more vulnerable groups, including those who are experiencing street homelessness.
City-based drug checking services and local early warning systems can also help to identify the local emergence of harmful substances. The government is also funding pilot projects that may provide technological and data driven innovations.
There remains a worrying lack of innovation in the response to non-opioid drugs such as benzodiazepines (544 deaths this year). Considering the high proportion of deaths attributed to long-term health conditions, it is essential that we continue to break down barriers to accessing timely healthcare in all its forms, including stigma and poor quality care.