The world has waited decades for a malaria vaccine, and now two have come along in quick succession. On October 2, the World Health Organization (WHO) recommended that a new malaria vaccine, R21, developed by the University of Oxford be rolled out for the prevention of malaria in children, just two years after another vaccine, the RTS,S, got its endorsement.
In this episode of The Conversation Weekly podcast, we find out why it’s been so hard to find a malaria vaccine – and hear from the scientists behind the new breakthrough.
In 2021, 619,000 people died from malaria, the majority of them children. The search for a vaccine has been underway for decades, but it’s particularly difficult due to the complexity of the malaria parasite.
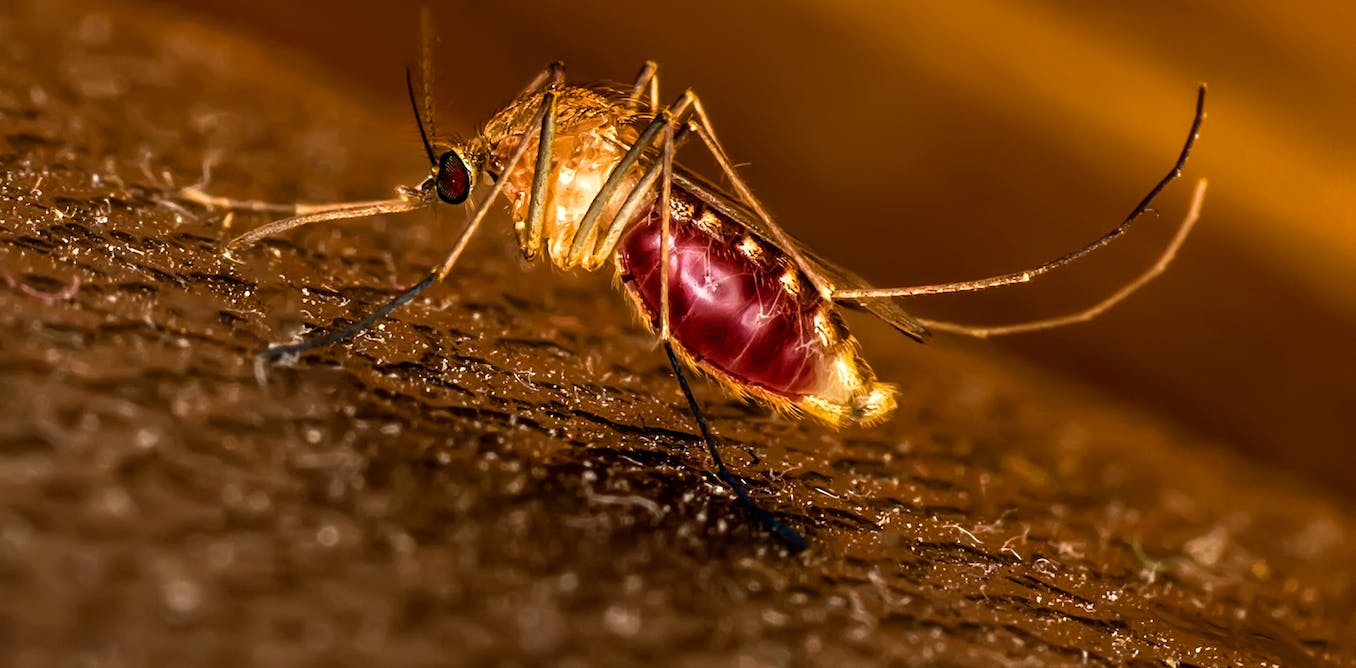
“It begins with a mosquito bite,” says Faith Osier, co-director of the Institute of Infection at Imperial College London. “It injects what we call sporozoite, a stage of the malaria parasite, that gets carried in your circulation into the liver and then it develops there”. About two weeks later, the parasites appear in the blood, morphing into different structures that are difficult to target with a vaccine.
But recent years have seen big breakthroughs in understanding what works. The RTS,S vaccine, which was developed by GSK, has been given to 1.7 million children in Ghana, Kenya and Malawi since 2019.
In early October 2023, the WHO recommended the use of a second malaria vaccine, created by the University of Oxford, called R21, following the publication of results from phase III clinical trials on children in Africa in a pre-print in The Lancet medical journal.
“We’re seeing about 75% efficacy of our vaccine,” says Adrian Hill, director of the Jenner Institute at the University of Oxford, which developed the new R21 vaccine. This means the vaccine can diminish “the number of clinical episodes that a child in Africa would get by 75%, compared to children who have not been vaccinated”.
Alassane Dicko, a professor at the Malaria Research and Training Center at the University of Bamako in Mali, conducted one of the stages of the phase III trial. He told The Conversation Weekly that in some of the most vulnerable groups in their trial, babies between five and 17 months, “the efficacy was 80%” after 12 months.
For comparison, the RTS,S vaccine showed around 55% efficacy after 12 months.
“It’s great to get higher efficacy, of course, but the big difference here with this vaccine is how you can manufacture it at a scale that is really needed to protect most of the children who need a malaria vaccine in Africa,” says Hill.
Oxford has been working with a partner, the Serum Institute of India, who it says has already established production capacity for 100 million doses a year. The higher volumes should also keep the cost of each dose relatively low.
To find out more about the vaccine, and what it means about the potential to fully eradicate malaria, listen to the full episode on The Conversation Weekly podcast.
This episode was written and produced by Katie Flood, with assistance from Gemma Ware and Mend Mariwany. Eloise Stevens does our sound design, and our theme music is by Neeta Sarl.
You can find us on Twitter @TC_Audio, on Instagram at theconversationdotcom or via email. You can also subscribe to The Conversation’s free daily email here.
Listen to The Conversation Weekly via any of the apps listed above, download it directly via our RSS feed or find out how else to listen here.