If you are a student in the UK, news of an outbreak of meningitis affecting university students in Kent may be causing you alarm.
The UK Health Security Agency has confirmed 13 cases of invasive meningococcal disease, a severe infection that can cause meningitis and septicaemia (blood poisoning), and is providing antibiotics and guidance to students and their close contacts. Two young people, a year 13 school pupil and a university student, have died. Others are seriously ill.
Why meningitis outbreaks happen at universities
Meningococcal disease is caused by Neisseria meningitidis bacteria. Although many people can carry the bacteria harmlessly in their nose or throat, very occasionally it invades the bloodstream or central nervous system and causes life-threatening illness. Meningitis is an inflammation of the membranes around the brain and spinal cord.
Meningococcal disease spreads through close contact with respiratory droplets. This could be through kissing, sharing drinks or utensils, and coughing and sneezing. This is what makes the risk higher in settings where people live, study and socialise closely together, such as university campuses.
Outbreaks such as the recent one in Kent, especially in communal settings like universities or schools, are less common than individual sporadic cases. While the overall risk remains low, the proportion of cases among young adults and students is higher than in older age groups simply because of the social mixing and living arrangements typical of school and university life.
How to reduce your risk
There is no guaranteed way to eliminate risk entirely, but several practical steps can help.
The first is vaccination. In the UK, there are routine immunisation programmes against key meningococcal strains. The MenACWY vaccine is usually offered in school to protect against four common meningococcal groups and can be given up to age 25 if missed. The MenB vaccine is given to infants. Whether older teenagers have had it varies because the risk profile and vaccine history differ. The MenB vaccine is available privately for teenagers and adults.
So check your vaccination history. You can do this by looking over your vaccination records, asking your GP practice, checking the NHS app or looking at your university or travel clinic records. If you can’t find a record of having a vaccination against meningitis, doctors may recommend vaccinating again – receiving an extra dose is generally safe.
Talk to your friends about their vaccination history, too. People can carry meningococcal bacteria without symptoms. Awareness of your own vaccination status and encouraging friends to be up to date increases community protection.
Even if someone has been vaccinated, they may still be advised to take preventive antibiotics if they were a close contact of a case of meningococcal disease.
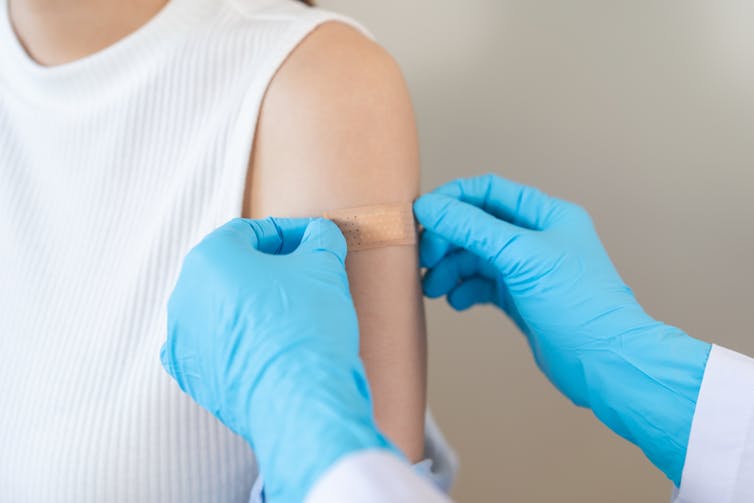
Kmpzzz/Shutterstock
Good hygiene is important. Simple measures like covering your mouth when coughing, not sharing drinks or utensils, washing hands regularly and avoiding close face to face contact when someone is ill can help reduce transmission.
What to look out for
One of the biggest challenges with meningococcal disease is that its early symptoms can look like flu or a bad cold, making it easy to overlook until it becomes severe. According to UK public health guidance, early symptoms can include fever or high temperature, a very bad headache, vomiting or nausea, muscle and joint pain, cold hands and feet, and rapid breathing. Symptoms can develop in different sequences and progress quickly.
As the disease progresses, more specific and serious “red flag” symptoms may appear. These include a stiff neck, confusion or delirium, dislike of bright lights, severe sleepiness or difficulty waking, seizures, and a rash that does not fade under pressure. This last is a key sign of septicaemia, and you can use the “glass test” to help identify it. Press a clear glass firmly against the glass. If it doesn’t fade under this pressure, contact a doctor straight away.
It’s crucial to stress that not all cases will show a rash, and no single symptom alone proves meningitis. But the combination of severe headache with fever, stiff neck, rash or rapid deterioration should prompt urgent suspicion.
If a friend shows symptoms
If you notice a friend exhibiting any concerning signs – especially rapid worsening over hours – take them seriously. Public health advice is clear: if symptoms are worrying or escalating, seek medical help immediately. In the UK, that means contacting NHS 111 for advice, or calling 999 if they are seriously unwell.
Check on your friend regularly, don’t dismiss symptoms as “just a hangover” and err on the side of urgency when in doubt. Early treatment with antibiotics can be lifesaving.
Acting quickly is vital
The Kent outbreak is a stark reminder that although meningococcal disease is uncommon, when it does occur it can progress rapidly and have devastating consequences. Students and young people, in particular, should be aware that illness can be serious even in previously healthy individuals. Early recognition and rapid medical response are vital and vaccination and awareness are primary tools for prevention.
While public health authorities work to contain outbreaks, the first line of defence is individuals and communities. Knowing the symptoms, acting quickly if someone becomes ill, and encouraging vaccination can make the difference between a contained case and a fatal outcome. In meningitis, the disease can escalate within hours. Early recognition and immediate action can save lives.
![]()
Manal Mohammed does not work for, consult, own shares in or receive funding from any company or organisation that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.



