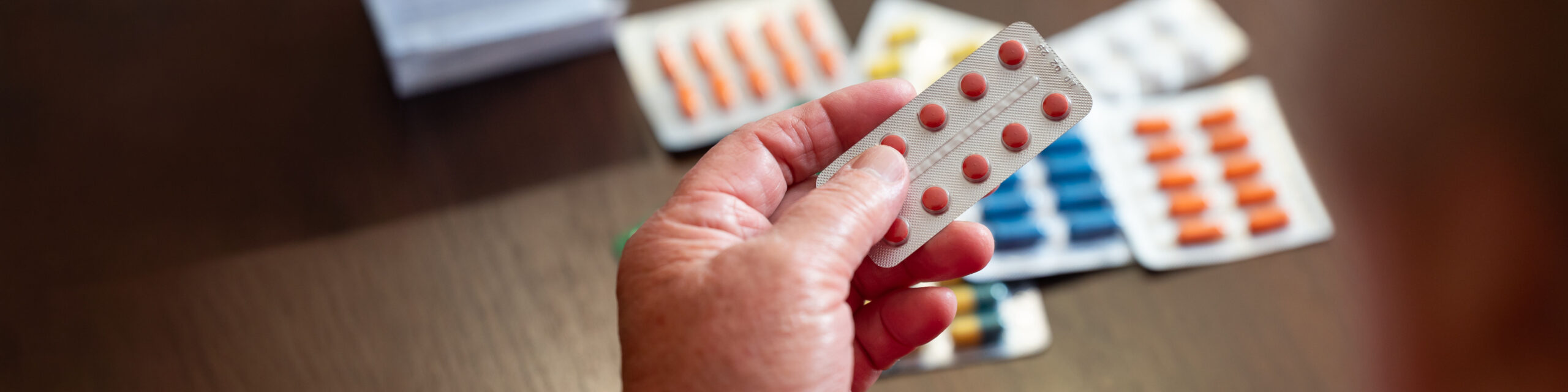
Over the past two decades, a wave of new drug treatments for rheumatoid arthritis (RA) has allowed many people to live free from pain, joint swelling and long-term disability. But for many patients in Europe, finding the right drug still involves months or even years of trial and error.
To change that, researchers, clinicians and patients from seven EU countries, plus Norway, Switzerland and the UK, have joined forces in an EU-funded initiative called SQUEEZE.
Rather than search for new RA drugs, their aim is to optimise the use of existing ones and find new biological clues to guide treatment, thus improving safety and efficacy for patients.
Professor Dr Daniel Aletaha from the Medical University of Vienna, who coordinates the five-year initiative, treats RA patients at a rheumatology centre in Vienna General Hospital.
“We have many effective therapies that can control rheumatoid arthritis, but we still don’t get enough patients into remission. The challenge is no longer only to develop new drugs – it is to maximise the impact of the ones we already have,” he explained.
A long road to the right treatment
RA is a chronic autoimmune condition in which the immune system attacks the joints, causing pain, stiffness, inflammation and fatigue.
“
The challenge is no longer only to develop new drugs – it is to maximise the impact of the ones we already have.
It often strikes people between the ages of 30 and 60, when they are busy raising families and building careers.
Without clear guidance on how a particular medicine will work for an individual patient, treatment decisions can feel like educated guesswork.
Patients may have to switch repeatedly from one medication to another, each time facing new worries about side effects and safety.
“That uncertainty is frustrating for patients and doctors alike,” said Aletaha.
Reaching remission faster – a period when symptoms are seriously reduced or disappear completely – means less pain, less fatigue and a lower risk of permanent joint damage.
From trial and error to precision care
A key focus for the SQUEEZE researchers is to identify biomarkers: measurable indicators of some biological state or condition which can help doctors select the right drug for the right person.
Researchers are analysing tissue samples from affected joints to see whether biomarkers at the site of inflammation can predict which therapy will be most effective for an individual patient.
They are also examining levels of the harmless but widespread torque teno virus in the blood, as a real-time indicator of how strongly a patient’s immune system is being suppressed.
Viral levels rise and fall depending on the intensity of treatment. Monitoring these levels could help doctors identify the sweet spot where drugs are powerful enough to control disease, but not so strong that they increase the risk of infection.
Optimising the dosage and delivery of drugs is another focus, to make sure each drug is used in the best possible way. Some studies in the project are examining whether patients in stable remission can safely reduce the dose of expensive biologic drugs, which would lower the risk of side effects and cut healthcare costs.
Others look at whether changing how a medicine is taken, such as injecting rather than swallowing methotrexate, can improve its effectiveness by increasing how much of the drug the body can absorb.
By pooling thousands of samples from across Europe, the researchers are building shared datasets that reflect diverse health systems.
“A person with rheumatoid arthritis is dealing with drugs, disease, human interactions with doctors, nurses – all that plays into a successful outcome,” said Aletaha.
The hidden barrier: taking medicines correctly
Even the most effective therapy cannot work unless taken as prescribed. Yet starting a treatment, taking it correctly and continuing it over time is a major challenge in chronic diseases.
Dr Agnes Kocher is part of Professor Dr Sabina De Geest’s team at the University of Basel in Switzerland. They are developing a digital, integrated care model that uses secure online tools to support patients between clinic visits. It also aims to shed light on why some patients go through so many drug switches.
“At the moment, as clinicians, if we see that the disease is not well controlled, we do not know if it’s because of the drug not working well, or whether adherence is the problem,” Kocher said.
The SQUEEZE care model combines medical and behavioural support to help patients better manage their medication in real-world settings.
Through electronic questionnaires linked to a national patient registry, the system identifies people at low, medium or high risk of non-adherence, and what is driving that risk. These factors range from fear of injections and troublesome side effects, to difficulty getting repeat prescriptions or keeping to a treatment regimen alongside other medicines.
The response is tailored to each patient and they receive ongoing support from the care team based on their level of risk and individual needs. A patient who skips a weekly dose because of a family event might be helped to adjust the timing. Someone anxious about injections may receive extra support from a specialist nurse.
Just as importantly, the model creates space for more open conversations. “Patients often tell us they don’t want to admit to their doctor that they struggle with treatment because they don’t want to be seen as a ‘bad patient’,” said Kocher.
The idea is that nurses may sometimes be better placed for patients to confide in, as they often spend more time with them and can build a more personal rapport.
Patients as partners
The Basel team hopes the new care model will improve doctor-patient conversations by helping doctors ask pertinent questions and enabling them to decide together on treatment changes.
“
Patients often tell us they don’t want to admit to their doctor that they struggle with treatment because they don’t want to be seen as a ‘bad patient’.
“Changing treatments creates a lot of uncertainty. There is the fear of returning to square one and their symptoms worsening under a new treatment, or more side effects, or running out of options.”
The contribution of people living with RA and patient groups is a striking feature of SQUEEZE.
“We have so many patients in this project, it’s very special,” said Kocher.
“When we see that the patients want to collaborate in our care model group because they really appreciate what we’re doing, it gives us a lot of energy.”
This care model is being co-created with patients, which makes it more acceptable, more realistic for everyday clinical practice and more likely to be used in the long run.
From project to practice
With clinical studies now under way and shared data from thousands of patients coming together, the SQUEEZE team expects to provide tools and training that help clinicians use biomarkers, dosing strategies and the new care model in everyday practice.
But for Aletaha, the ultimate goal is not a document. “Guidelines alone don’t change practice,” he said.
“Impact comes when the knowledge is actually used in clinics and improves people’s lives. We want every patient to get the treatment that works for them – as early as possible.”
Research in this article was funded by the EU’s Horizon Programme. The views of the interviewees don’t necessarily reflect those of the European Commission. If you liked this article, please consider sharing it on social media.