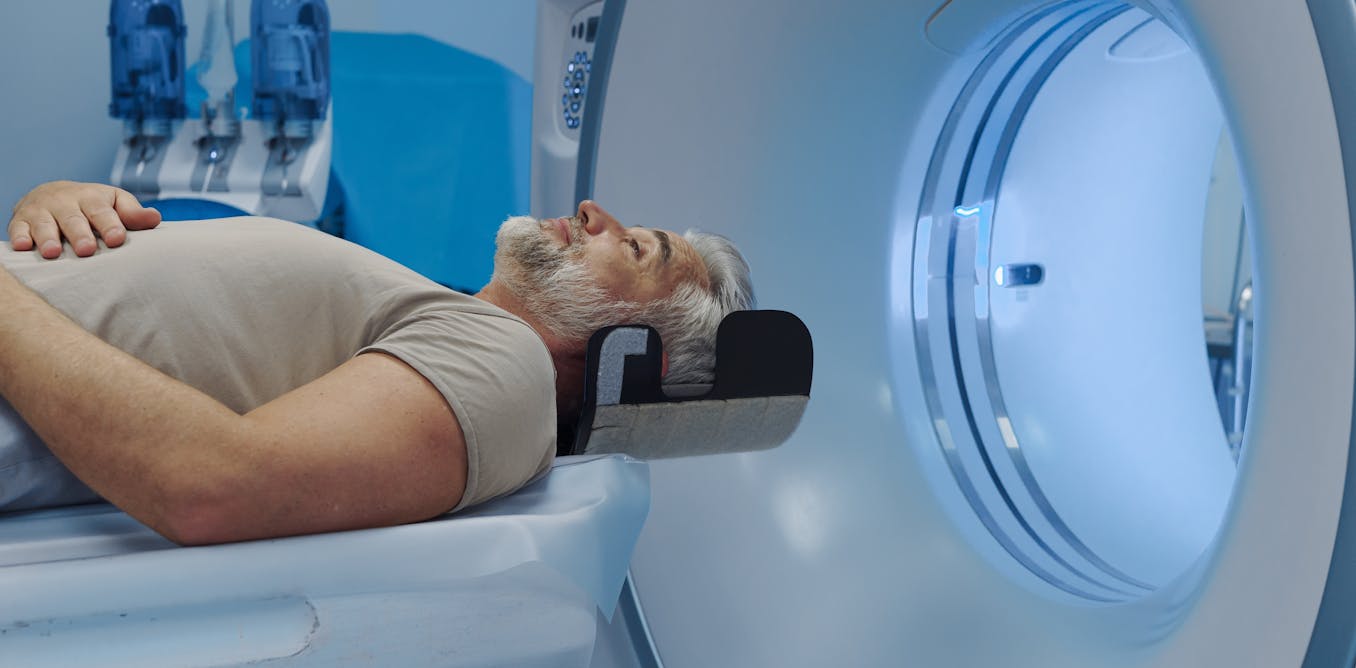
Weight-loss injections that have become famous for helping people shed pounds may also help some patients with advanced cancer live longer when the disease has spread to the brain, according to a new study.
These medicines belong to a group of drugs called GLP-1 receptor agonists, and they include Wegovy and Ozempic. They were first developed to treat type 2 diabetes, but over the past few years they have drawn global attention because many people taking them experience significant weight loss.
The new study does not show that these injections directly treat cancer. Instead, it suggests something more subtle but potentially important: they might help some very ill patients live longer.
The study focuses on brain metastases. This happens when cancer cells travel from somewhere else in the body – such as the lung, breast or skin – to form tumours in the brain. Unfortunately, brain metastases are relatively common and usually indicate that cancer has reached a late and dangerous stage.
Many patients in this situation also have type 2 diabetes. This matters because the condition can make serious illness harder to manage. High blood sugar can cause chronic inflammation, damage blood vessels and weaken the body’s ability to cope.
In my own clinical practice, I often prescribe steroids to help patients with brain metastases manage symptoms such as swelling in the brain. Steroids can be very effective, but they also tend to raise blood sugar levels and can make diabetes harder to control. This has led researchers to ask whether GLP-1 drugs might have additional benefits.
When diabetes drugs meet cancer care
Laboratory studies suggest they may protect brain cells, reduce inflammation and help preserve the brain’s blood supply. Until now, however, there has been very little evidence from everyday clinical practice showing how patients with both diabetes and brain metastases fare when they take these medicines.
The new study, published in Jama Network Open, set out to explore that question. Researchers used a medical database of anonymised health records from 151 hospitals and healthcare systems around the world.
They searched for adults who had three conditions: cancer, type 2 diabetes and brain metastases. The records covered patients seen between 2018 and 2024. The researchers were particularly interested in whether these patients had been prescribed a GLP-1 drug – such as semaglutide, dulaglutide, liraglutide or tirzepatide – around the time their diabetes and brain metastases were first diagnosed.
Rebel Red Runner/Shutterstock.com
To make a fair comparison, the team matched people who received one of these injections with similar patients who did not. They took into account factors such as age, sex, type of cancer, other medical conditions and treatments including chemotherapy, radiotherapy and steroid use. Statistical matching cannot eliminate every difference between groups, but it helps reduce the risk that the results simply reflect one group being healthier at the start.
In total, the researchers identified more than 19,000 patients with cancer, brain metastases and type 2 diabetes. Among them, 866 had been treated with a GLP-1 drug, while over 11,000 had not. After careful matching, the analysis compared two balanced groups of 850 patients each who were similar in terms of their cancers, body mass index, diabetes control and other health issues.
The researchers then followed these patients for up to three years after their brain metastases were first recorded. Their main question was straightforward but important: how many people in each group died during that period?
The researchers found that patients who were taking GLP-1 drugs were significantly less likely to die during the follow-up period than those who were not. Overall, people taking GLP-1 drugs were about 37% less likely to die over the three years.
The pattern was fairly consistent across several major cancer types, including lung cancer, breast cancer and melanoma. It also appeared across different drugs within the GLP-1 class.
When researchers compared GLP-1 medicines with other modern diabetes treatments – including drugs called SGLT2 inhibitors and DPP-4 inhibitors – the GLP-1 group still seemed to fare better. That hints that something about GLP-1 signalling itself might be beneficial, rather than the effect simply coming from better blood sugar control.
Important limitation
Even so, the researchers emphasise an important limitation. This study looked back at medical records rather than testing treatments in a controlled trial. To do that, researchers would need randomised clinical trials in which patients are deliberately assigned to receive a GLP-1 drug or another treatment and then followed over time.
So how might these so-called weight-loss jabs help people whose cancer has spread to the brain?
One possibility is that they help indirectly by improving diabetes itself. Better blood sugar control, reduced body weight and improved heart health could help patients cope better with surgery, radiotherapy or chemotherapy.
But there may also be more direct effects on the brain. Scientists have discovered that GLP-1 receptors are in brain tissue and play a role in controlling inflammation, protecting nerve cells and helping maintain the blood–brain barrier – a protective layer that keeps harmful substances out of the brain.
Animal studies suggest that activating these receptors can reduce damage in brain cells and help them function properly. In theory, that might help the brain tolerate metastatic tumours better or make it a less favourable environment for cancer cells to grow. The new clinical findings are consistent with these ideas, although they do not yet tell us which mechanisms matter most in people.
For patients and families reading about this research, it is important to understand what the results do – and do not – mean. The study does not suggest that people with brain metastases should rush to start GLP-1 drugs, nor that these medicines can replace standard cancer treatments such as radiotherapy, surgery, targeted therapies or immunotherapy.
The potential benefits were seen specifically in people who already had type 2 diabetes. Like any medication, these injections can cause side-effects such as nausea and vomiting, and there are ongoing discussions about rare but serious risks.
Anyone considering them would need careful guidance from both their oncology and diabetes teams rather than making decisions based on a single study.
Still, the findings open up an intriguing new line of research linking cancer, metabolism and brain health. If future trials confirm that GLP-1 drugs genuinely improve survival in patients with brain metastases and diabetes, they could eventually become part of supportive care for people facing this difficult complication.
![]()
Justin Stebbing does not work for, consult, own shares in or receive funding from any company or organisation that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.