For years, debates about maternity care have centred on how women give birth. But the more important question has always been safety.
Vaginal birth, assisted birth and caesarean section are different clinical routes, not measures of success. The outcome that matters is the wellbeing of both mother and baby, guided by individual risk and informed decision making.
In the wake of maternity investigations, public debate has focused on staffing levels, organisational culture and accountability. These are essential concerns. But there is another, less visible issue. We still do not fully measure or understand what physically happens during childbirth itself.
Labour is one of the most physically demanding processes the human body experiences. It involves coordinated muscle activity, shifting pressure through the pelvis and spine, and joints adapting under intense physiological stress. Yet there are currently no studies directly measuring how labour positions, movement, hands-on techniques and physical forces affect the mother and baby in real time during active labour.
As a result, many positioning strategies are based largely on tradition and accumulated clinical experience rather than direct measurement.
Guidance sometimes suggests certain positions are better than others. But bodies do not behave in one-size-fits-all ways. Research examining upright birthing positions shows there is no single ideal mechanical pattern. The same position can distribute strain differently depending on flexibility, spinal curvature, previous injury and joint mobility.
Despite this complexity, active labour is still not measured biomechanically in real time, while other demanding physical activities have been studied in great detail. Marathon running, for example, has been analysed extensively. Researchers have mapped muscle activity, joint forces and how the body interacts with the ground. Birth has not received the same level of mechanical study.
Read more:
Why we still don’t understand what happens to women’s bodies during labour
This gap reflects long-standing research priorities. Women were historically excluded from large areas of clinical research, and funding for women’s health remains comparatively limited. In England, a dedicated Women’s Health Strategy was introduced only in 2022.
Foetal movement
One of the most common reasons women seek urgent maternity assessment is reduced or absent foetal movement. Yet foetal movement itself is not directly measured.
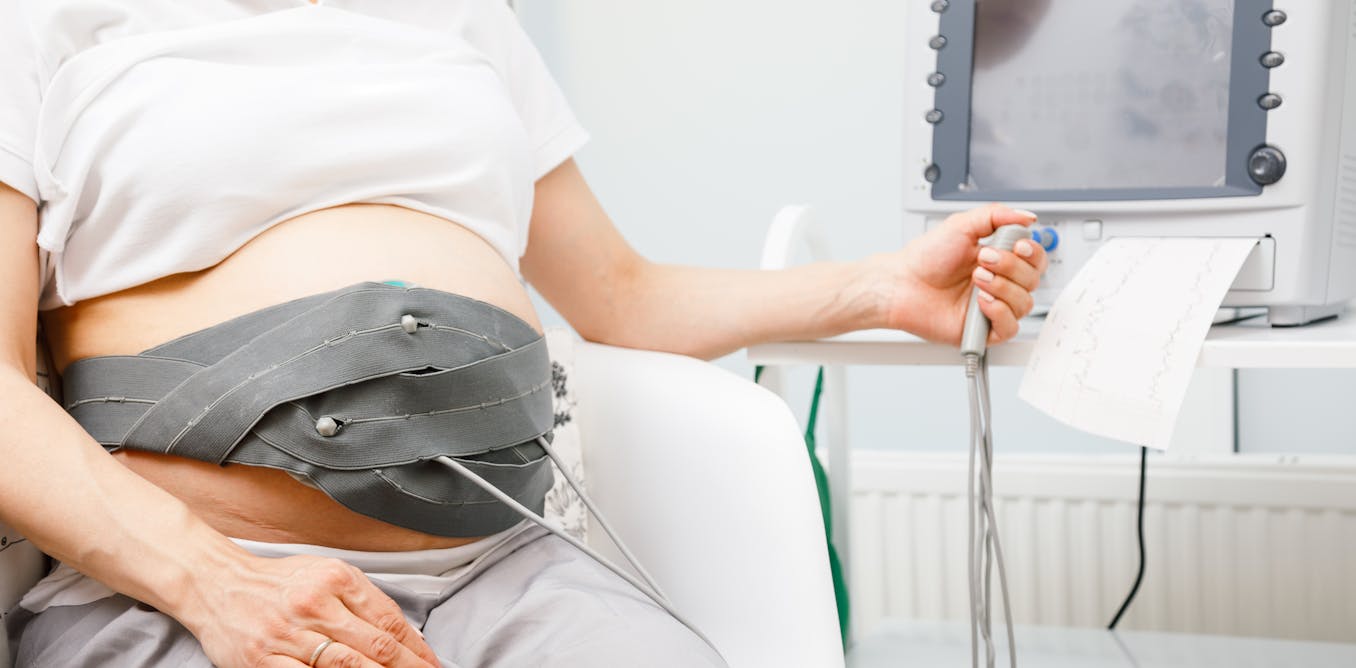
The main monitoring tool used in pregnancy and labour is cardiotocography, often called CTG. It tracks the baby’s heart rate and the mother’s contractions. It does not capture how the baby moves, such as limb activity, rotation or developing movement patterns. In practice, assessment still relies largely on what the pregnant woman feels and reports.
When someone says, “My baby is not moving normally,” she is describing a change we cannot objectively measure in real time. If detecting change early is central to safe care, this gap matters. When reassurance is given, it is based on the measurements we currently have, but not always the ones we need.
The education gap
Midwives, obstetricians and maternity teams support one of the most physically demanding processes the human body undergoes. Yet formal education in biomechanics is limited. Biomechanics is the study of how forces move through the body, how joints interact and how changing one angle affects another.
Understanding how altering hip position affects the pelvis and spine is not abstract theory. It can influence comfort, pressure on tissues and potentially safety.
Embedding biomechanics into maternity education is not about criticising clinicians. It is about giving them more precise tools and knowledge to support decision making.
Improving maternity safety requires care to be guided by evidence rather than shaped mainly by tradition.
The NHS spends substantial sums each year on maternity-related negligence payments. Investing even a fraction of this in rigorous childbirth research, alongside improvements to staffing and systems, could strengthen the scientific foundation of care and support safer, more personalised decisions.
Behind every statistic is a family living with loss, trauma or unanswered questions. Improving maternity safety is not only about accountability or workforce pressures. It is also about understanding what happens during labour, equipping clinicians with better knowledge and ensuring women’s concerns are supported by reliable tools.
Birth is one of the most significant physical events in human life. It deserves to be studied and understood with the same scientific rigour applied to any other complex medical process.
![]()
Anastasia Topalidou received funding from the NIHR Applied Research Collaboration North West Coast (NIHR ARC NWC) for the completion of the scoping review referenced in this article.